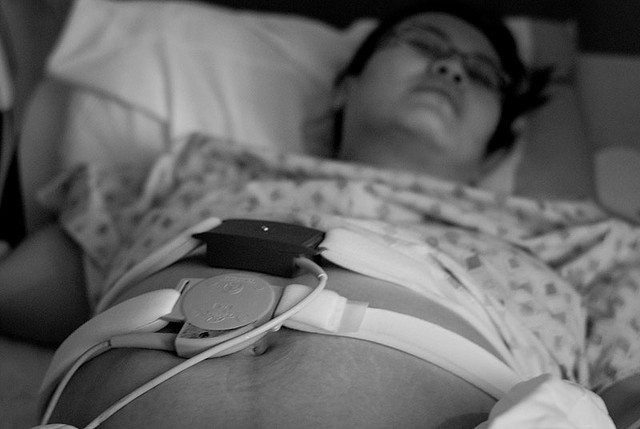
Babies with hypoxic-ischemic encephalopathy (HIE) are often born to mothers who had high-risk pregnancies. Women with high-risk pregnancies should receive extra prenatal monitoring and care; if a physician fails to recognize that a pregnancy is high-risk or provides inadequate care, this can put the health of both the mother and baby at risk (1).
In order to prevent HIE and other neonatal complications, it may be necessary to conduct frequent testing. These tests may include non-stress tests (NSTs), which ensure that the baby’s heart rate is reacting normally to their movement, biophysical profiles (BPP), which include both a non-stress test and a fetal ultrasound, and Doppler flow studies.
What makes a pregnancy high-risk?
A high-risk pregnancy is any pregnancy that has risk factors for the mother or baby developing a serious health issue. Some women are at increased risk before getting pregnant, while other women develop a high-risk pregnancy over time .There are many factors that can make a pregnancy high-risk, including the following (2):
- Maternal obesity and high BMI
- Diabetes and gestational diabetes
- High blood pressure
- Preeclampsia
- Multiparous birth (multiples)
- Immune disorders
- Alcohol and tobacco use during pregnancy
- Advanced maternal age or young maternal age
- History of placental abruption or preterm birth
- Intrauterine growth restriction (IUGR)
- Neural tube defects
- Previous cesarean delivery
- Previous stillbirth
- Neonatal heart problems
Just because a pregnancy is classified as high-risk does not necessarily mean that the child will have a birth injury like hypoxic-ischemic encephalopathy. Often, HIE stems from medical staff not recognizing a high-risk pregnancy when they should have, or failing to provide sufficient monitoring and care to a woman with a high-risk pregnancy. High-risk pregnancies must be properly monitored to allow the parents and doctors to work together to mitigate the risks.
Maternal obesity and high BMI
Obesity is defined as having a body mass index (BMI) of 30 or greater. This can be a delicate subject because weight loss can be difficult for patients. Sometimes, physicians gloss over the health risks related to obesity because the topic is a challenging one to broach, but it is necessary to discuss due to the accompanying risks.
Women who have a very high BMI have a higher risk of having gestational diabetes, hypertension (high blood pressure), preeclampsia, premature birth, and pregnancy loss (3). There is also a risk that babies can be macrosomic (far larger than expected), which can make labor difficult. Alternatively, there are also cases where the babies of women with a very high BMI have a condition called intrauterine growth restriction (IUGR), which means that the baby is smaller than normal for their gestational age. Babies with IUGR tend to tolerate labor poorly and are at a higher risk of brain bleeds. Despite these risks, it is very possible to have a healthy pregnancy when a woman is overweight. The important thing is that your doctors monitor you more closely during pregnancy and delivery (3).
Diabetes and gestational diabetes
Diabetes is a condition that should be properly controlled and monitored for both the health of mother and child. In some cases, diabetes can be first diagnosed during a pregnancy. This type of diabetes is called gestational diabetes. Uncontrolled or poorly managed diabetes can cause health problems in the mother, but also poses a health risk for the fetus, because the baby can become macrosomic (very large), prolonging labor (4). Due to their size, it is also more likely that a macrosomic baby will get their shoulders stuck on the mother’s pelvis, increasing their risk of a condition called Erb’s palsy, which is damage to the brachial plexus nerves. When a baby gets stuck in the birth canal, this is also a direct factor that influences the baby’s risk of hypoxic-ischemic encephalopathy. Finally, gestational diabetes increases the risk of preeclampsia, hypoglycemia, and cesarean delivery (4).
High blood pressure
High blood pressure, or hypertension, occurs in roughly one in 12-17 pregnancies between the ages of 20 and 44 in the U.S. High blood pressure during pregnancy can lead to the following (5):
- Preeclampsia
- Eclampsia
- Stroke
- Placental abruption
- Low birth weight
- Preterm birth
- Hypoxic-ischemic encephalopathy*
*Mothers and babies are connected to each other via the placenta and umbilical cord, which provide a constant flow of nutrients and oxygen to the baby. These nutrients and oxygen are carried to the baby through the blood. Blood flow is regulated by numerous factors, but one of the most important factors is blood pressure. Very low or very high blood pressure can compromise the free flow of blood between the two, and creates a risk for the baby to suffer oxygen deprivation, or hypoxic-ischemic encephalopathy (HIE).
As a result of all of the above-mentioned risks associated with high blood pressure during pregnancy, it is imperative that the pregnancy be monitored closely.
Preeclampsia
Preeclampsia is a subtype of high blood pressure, but it is specifically high blood pressure that is first diagnosed during a pregnancy (5). Women who had hypertension before pregnancy can also develop preeclampsia. A woman has preeclampsia if she develops high blood pressure and protein in her urine after 20 weeks of gestation (5). Preeclampsia occurs in approximately 5-8% of pregnancies. It is marked by severe headaches, changes in vision, nausea/vomiting, stomach pain, swelling in the face or hands, difficulty breathing, and sudden weight gain (5). It is possible for a woman not to experience or be able to differentiate her symptoms from normal pregnancy symptoms. For this reason, it is imperative that the doctor checks her blood pressure and urine sample at every prenatal visit.
If not treated and monitored properly, preeclampsia can cause maternal liver or renal failure, as well as subsequent cardiovascular issues (6). It can also lead to eclampsia, which is a condition where the mother has seizures. An additional risk is HELLP Syndrome, a condition that affects maternal liver function and blood flow.
How does preeclampsia affect the baby?
Preeclampsia can also prevent the placenta from getting the blood it needs (6). If the placenta doesn’t get enough blood, the baby doesn’t get enough oxygen or food. This can result in hypoxic-ischemic encephalopathy (HIE) or low birth weight, as well as other complications. Because preeclampsia is an exceptionally risky condition (and because it can progress from mild to severe very quickly), physicians deliver babies prior to term to protect both the mother and the baby.
Multiparous births (multiple births)
Having multiples is a joyous occasion, but also requires some additional monitoring on the part of doctors. Multiple births are common, making up 3 in 100 births and rising (7). Multiple pregnancies in general have increased over the last few decades, for many reasons. Women over age 35 are at a higher chance of having multiples, and more women in this age group are giving birth (8). Additionally, more women in this age group undergo fertility treatments to get pregnant, which increases the chances of multiples.
Babies born in multiples are at greater risk of complications, and this risk increases the more babies that are in a group (8). Babies born in multiples are at a greater risk for premature birth, with more than 50% of twins and more than 90% of triplets being born prematurely. Premature birth is associated with a greater risk of complications, including HIE, cerebral palsy (CP), and other disabilities.
Immune disorders (HIV/AIDS)
Mothers with HIV are considered to be high-risk, as this population must be monitored and treated properly to reduce the risk of transmitting HIV to their child (9). Medical staff must inform mothers with HIV of advised steps, such as taking ART (antiretroviral therapy) and having a C-section rather than a vaginal birth. After birth, there are certain steps that doctors must take, such as advising mothers not to breastfeed and to follow treatment plans closely.
Alcohol and tobacco use during pregnancy
It is the responsibility of medical staff to inform mothers who use alcohol and tobacco about the risks of substance use during pregnancy, as this can negatively affect the baby’s growth and development (10). Maternal alcohol consumption hinders normal fetal growth and puts infants at risk for fetal alcohol syndrome (FASD), which is known to cause intellectual disabilities and developmental delays. Smoking is associated with intrauterine growth restriction (IUGR), preterm birth, and other long-term health difficulties. It also increases the infant’s risk of sudden infant death syndrome (SIDS). Physicians must inform pregnant patients who smoke of smoking cessation programs. Smoking cessation programs have been proven to help patients quit smoking.
Advanced or young maternal age
Women who get pregnant after the age of 35 are considered to be of advanced maternal age. This puts them at a higher risk of various pregnancy complications, including multiples, gestational diabetes, premature birth, a low birth weight baby, high blood pressure, C-section delivery, and others (11). Pregnancy before age 20 is also associated with increased risks, including preterm birth, chorioamnionitis, preeclampsia, poor fetal growth, fetal distress, postpartum hemorrhage, and others (12).
History of placental abruption or preterm birth
Having experienced certain things in a previous pregnancy can put you at an increased risk of experiencing them again down the line. This happens with placental abruption, a condition which has a very high rate of recurrence (13). The possibility of it happening in subsequent pregnancies is so high, in fact, that elective induction at 37 weeks is advised for women with a previous placental abruption. Preterm birth is another condition that can be recurrent, depending on what caused the previous preterm birth (14). Certain demographics are more likely to experience recurrent preterm births, as well. Preterm births increase the risk of birth injuries, such as HIE, cerebral palsy, cognitive disabilities, and others.
Intrauterine Growth Restriction (IUGR)
Intrauterine growth restriction (IUGR), often referred to as fetal growth restriction, occurs when the baby is too small for their gestational age. This can happen as a result of maternal health issues, fetal health issues, or placental or uterine issues. Infants who are born small are at a higher risk of many complications, including (but not limited to) premature birth, hypoxic-ischemic encephalopathy (HIE), hypoglycemia, impaired immune function, and impaired thermoregulation (15). Because of the many complications associated with IUGR, it is considered a high-risk condition, requiring extra monitoring. Tests such as weight checks, non-stress tests (NSTs), biophysical profiles, amniotic fluid index, and doppler velocimetry tests should be administered to assess the wellbeing of the infant. The mother may be referred to a maternal-fetal medicine specialist. Severely growth-restricted babies should be delivered in a perinatal center with medical professionals who are experienced in perinatal asphyxia, HIE, pulmonary hypertension, meconium aspiration, and hypoglycemia (15). Prompt delivery should always be considered, and IUGR babies are almost always born before term.
Neural tube defects
Neural tube defects (NTDs), such as spina bifida and anencephaly, are birth defects of the brain and spinal cord. NTDs occur in roughly 3,000 pregnancies per year in the U.S. (16). In these cases, the neural tubes in certain areas don’t close completely, causing severe complications. In the case of spina bifida, part of the spinal cord pokes through the spine, which can result in issues with controlling bladder or bowel movements, paralyzation of the legs, and other risks. If your baby is diagnosed with an NTD during pregnancy, certain health treatments can be implemented. You may be advised to deliver the baby in a hospital that specializes in NDTs, have surgery for spina bifida in the womb, or deliver in a certain way to protect the baby (vaginal or cesarean) (16).
Previous or multiple cesarean deliveries
Women who have had one or more cesarean deliveries in the past are at an increased risk of maternal hemorrhage, or heavy bleeding. The risks of hysterectomy, bladder and bowel injuries, and problems with the placenta also increase with the number of cesarean deliveries a woman has (17). Because of this, your doctor should monitor your pregnancy closely if you have previously had a C-section delivery.
Previous stillbirth
A pregnancy following a stillbirth (the death of a baby after 24 weeks gestation) falls into the “high risk” category. This is because people who have had a stillbirth before are at a higher risk of having another one. There are many contributing factors to this, including whether or not the cause of the stillbirth was identified, whether other high-risk conditions are present, etc. (18). It is likely in any event that the medical professional will request extra monitoring after a stillbirth.
Neonatal heart problems
If your baby is born with a heart defect, this can affect future pregnancies. The risk of having a baby with a congenital heart defect (CHD) is roughly 1%. The risk of having another baby with a CHD depends on the child’s specific diagnosis, but is in the range of 2-3%. In order to manage these high-risk pregnancies more closely, doctors may recommend meeting with a genetic counselor and a maternal fetal medicine specialist, as well as getting a fetal echo between 18 and 24 weeks in all future pregnancies (19). The delivery should be planned carefully and done in a hospital with appropriate neonatal care facilities.
About the HIE Help Center
The HIE Help Center is run by ABC Law Centers (Reiter & Walsh, P.C.), a medical malpractice firm exclusively handling cases involving HIE and other birth injuries that may have resulted from undiagnosed high-risk pregnancy complications or mismanaged high-risk pregnancy. Our lawyers have over 100 years of combined experience with this type of law, and have been advocating for children with HIE and related disabilities since the firm’s inception in 1997.
We are passionate about helping families obtain the compensation necessary to cover their extensive medical bills, loss of wages (if one or both parents have to miss work in order to care for their child), assistive technology, and other necessities.
If you suspect your child’s HIE may have been caused by medical negligence, please contact us today to learn more about pursuing a case. We provide free legal consultations, during which we will inform you of your legal options and answer any questions you may have. Moreover, you would pay nothing throughout the entire legal process unless we obtain a favorable settlement.
You are also welcome to reach out to us with inquiries that are not related to malpractice. We cannot provide individualized medical advice, but we’re happy to track down informational resources for you.
Sources
- High-risk pregnancy: Know what to expect. (2018, February 21). Retrieved December 14, 2019, from https://www.mayoclinic.org/healthy-lifestyle/pregnancy-week-by-week/in-depth/high-risk-pregnancy/art-20047012.
- What is a high-risk pregnancy? (2017, January 31). Retrieved December 14, 2019, from https://www.nichd.nih.gov/health/topics/pregnancy/conditioninfo/high-risk.
- Obesity and Pregnancy. (2016, April). Retrieved December 14, 2019, from https://www.acog.org/Patients/FAQs/Obesity-and-Pregnancy?IsMobileSet=false.
- Gestational Diabetes and Pregnancy. (2019, October 28). Retrieved December 14, 2019, from https://www.cdc.gov/pregnancy/diabetes-gestational.html.
- High Blood Pressure During Pregnancy. (2019, June 20). Retrieved December 21, 2019, from https://www.cdc.gov/bloodpressure/pregnancy.htm.
- Preeclampsia: Symptoms, Risks, Treatment and Prevention. (2019, October 9). Retrieved December 21, 2019, from https://americanpregnancy.org/pregnancy-complications/preeclampsia/.
- default – Stanford Children’s Health. (n.d.). Retrieved January 24, 2020, from https://www.stanfordchildrens.org/en/topic/default?id=overview-of-multiple-pregnancy-85-P08019
- ACOG. (n.d.). Multiples: When It’s Twins, Triplets, or More. Multiples: When It’s Twins, Triplets, or More.
- Women’s Health Care Physicians. (2017, July). Retrieved January 22, 2020, from https://www.acog.org/Patients/FAQs/HIV-and-Pregnancy?IsMobileSet=false
- Women’s Health Care Physicians. (2019, February). Retrieved January 22, 2020, from https://www.acog.org/Patients/FAQs/Tobacco-Alcohol-Drugs-and-Pregnancy?IsMobileSet=false
- Pregnancy after 35: What you need to know. (2017, August 5). Retrieved February 7, 2020, from https://www.mayoclinic.org/healthy-lifestyle/getting-pregnant/in-depth/pregnancy/art-20045756
- Cavazos-Rehg, P. A., Krauss, M. J., Spitznagel, E. L., Bommarito, K., Madden, T., Olsen, M. A., … Bierut, L. J. (2015). Maternal age and risk of labor and delivery complications. Maternal and child health journal, 19(6), 1202–1211. doi:10.1007/s10995-014-1624-7
- Ruiter, L., Ravelli, A. C. J., de Graaf, I. M., Mol, B. W. J., & Pajkrt, E. (2015, October). Incidence and recurrence rate of placental abruption: a longitudinal linked national cohort study in the Netherlands. Retrieved February 7, 2020, from https://www.ncbi.nlm.nih.gov/pubmed/26071916
- Mazaki-Tovi, S., Romero, R., Kusanovic, J. P., Erez, O., Pineles, B. L., Gotsch, F., … Hassan, S. S. (2007). Recurrent preterm birth. Seminars in perinatology, 31(3), 142–158. doi:10.1053/j.semperi.2007.04.001
- (n.d.). Retrieved August 23, 2018, from https://www.uptodate.com/contents/infants-with-fetal-intrauterine-growth-restriction
- Neural tube defects. (n.d.). Retrieved February 7, 2020, from https://www.marchofdimes.org/complications/neural-tube-defects.aspx
- Repeat C-sections: Is there a limit? (2018, June 8). Retrieved February 7, 2020, from https://www.mayoclinic.org/tests-procedures/c-section/expert-answers/c-sections/faq-20058380
- Danielsson, K. (2018, November 23). Discussing With Your Partner to Try for Another Baby After Stillbirth. Retrieved February 7, 2020, from https://www.verywellfamily.com/when-is-it-safe-to-conceive-after-stillbirth-2371776
- Future Pregnancy After CHD Diagnosis: 3 Things To Know. (2019, April 17). Retrieved February 7, 2020, from https://blog.cincinnatichildrens.org/rare-and-complex-conditions/heart-conditions/future-pregnancies-after-chd-diagnosis-3-things-to-know